What Does a Low Creatinine Level Mean in a Premature Baby
Abstract
Objectives:
Piffling is known about the human relationship between gestational age (GA) or birth weight (BW) and serum creatinine (SCr) in very low birth weight (VLBW) infants. We sought to report postnatal SCr changes and determine if there is a correlation between GA or BW and SCr in VLBW infants, during their kickoff days of life.
Study Design:
Medical records of all VLBW infants, who were admitted to our neonatal intensive care unit of measurement (NICU) between 1 May 1998 and 1 May 2001, were reviewed. Medical records were reviewed for: BW, GA, gender, race, APGAR scores, mechanical ventilation, use of medications, fluid intake, urinary output, poly peptide intake, blood urea nitrogen (BUN) and SCr during the beginning days of life. Patients with anuria/oliguria, major congenital anomalies, low APGAR scores at 5?min, on high ventilator settings (on the oscillator), hemodynamically unstable (on pressors, inotropes) and on indomethacin and diuretics were excluded.
Results:
In full, 138 infants met our inclusion criteria. SCr was found to subtract postnatally, reaching a plateau on solar day five of life in all VLBW infants (repeated measure analysis of variance; P=0.004); nevertheless, in that location was a delay in the subtract of SCr in the subgroup of infants <29 weeks GA, and <1000?g BW. SCr (on day 5 of life) was likewise establish to decrease with increasing GA and BW (Pearson correlation coefficient: −0.206 (P=0.05) and −0.236 (P=0.05) respectively).
Decision:
In VLBW infants SCr decreases significantly during the start days of life; however, in infants younger than 29 weeks GA or smaller than 1000?thousand BW at that place is a delay in the decrease of their SCr that extends across the offset days of life. We also conclude that during the offset days of life, and in VLBW infants SCr decreases with advancing GA and BW.
Introduction
Renal office is immature in very low birth weight (VLBW) and premature infants as compared to adults,1 and serum creatinine (SCr) in newborn infants is elevated during the offset week of life.2, 3, iv While in the firsthand postnatal period the newborn SCr likely reverberate maternal values,2, 4 farther increase in the levels of SCr in premature infants have been attributed to increased tubular reabsorption of creatinine due to renal tubular immaturity and also to reduced creatinine clearance.2, 3
It has likewise been shown by several investigators that creatinine clearance and glomerular filtration charge per unit (GFR) increment with postnatal historic period in premature infants,5, six, 7, 8 and in the absence of urine creatinine measurements, SCr can exist used to guess GFR.9, 10, 11, 12 Nonetheless, little is known about the relationship between gestational age/birth weight (GA/BW) and SCr in VLBW infants at birth following stabilization of their SCr.
This study was conducted to determine postnatal SCr changes in VLBW infants and to decide if at that place is a correlation between GA or BW and SCr in VLBW infants, during their first days of life.
Patients and methods
Patients
Medical records of all VLBW infants (⩽1500?yard at nascency) admitted to our neonatal intensive care unit (NICU) between 1 May 1998 and 1 May 2001 were identified by searching our electronic data base program. Medical records were reviewed for: GA, BW, length at birth, gender and race. Medical records were as well reviewed for APGAR scores at 5 and 10?min of age, mechanical ventilation, continuous positive airway pressure (CPAP), daily fluid intake, urinary output, protein intake, blood urea nitrogen (BUN) and SCr during the outset half-dozen days of life. Patients who were on the oscillator, and who received dopamine, dobutamine, indomethacin, gentamicin, xanthines (aminophylline, caffeine) and diuretics were also identified.
Morning laboratory values were analyzed and hemolyzed samples were excluded. Hemolyzed samples were identified by the laboratory technicians. Morning laboratory values were collected during the starting time calendar week of life between day two and half dozen. Mean solar day 2 of life was considered the first morning afterward the kickoff 24?h of life.
Our inclusion criteria consisted of all VLBW infants who were admitted to our NICU during the study period.
Our exclusion criteria consisted of all patients with anuria/oliguria, patients on indomethacin, amphotericin and diuretics, patients on high ventilator settings (on the oscillator), patients hemodynamically unstable on pressors and or inotropes (epinephrine, dobutamine and dopamine) and patients with major congenital anomalies. Patients with a depression five?min APGAR score (<5) were also excluded.
Anuria was defined as a 24?h urinary output boilerplate of <one?ml/kg/h during the first six days of life. SCr was adamant by the Jaffe method, using the SYNCHRON Sixty 20 system.13
The study was canonical past our Institutional Review Board at MetroHealth Medical Center.
Statistical assay
A repeated measure out analysis of variance (ANOVA) was used to make up one's mind the deviation of SCr, BUN, intravenous fluid intake and urinary output of all VLBW infants over time (during the offset 6 days of life). A paired t-exam (with Bonferroni correction) was used for comparison between different days (2, three, 4 and 5) and twenty-four hour period vi of life. A Pearson test was used for correlation analysis between SCr and GA. A Pearson test was also used for correlation analysis betwixt SCr and BW. Values were expressed as mean±s.d. or every bit mean±due south.e. of the hateful. P<0.05 was considered statistically significant. For nominal data the χ 2-exam was used. To adjust for possible confounding, a logistic regression assay was used. Variables known to modify SCr were entered in a logistic regression model using a subtract past ⩾10% of SCr between mean solar day 2 and 6 of life equally a classifying and dependent variable.
Results
During the study period, 1977 newborn infants were admitted to our NICU. 20 eight per centum (547/1977) were ⩽32 weeks GA. However, only 138 infants met our inclusion criteria. The demographics of the 138 infants are summarized in Tabular array 1.
SCr decreased in VLBW infants during their first days of life (repeated mensurate ANOVA; P=0.004, n=138. Figure 1a), and in that location was a statistically significant differences (t-test with Bonferroni correction) between SCr on twenty-four hours ii and 6 (0.75±0.22 versus 0.67±0.22, respectively; P<0.001), and twenty-four hour period iii and 6 (0.75±0.24 versus 0.67±0.22, respectively; P=0.001). However, there was no departure betwixt SCr on day 4 and half dozen (0.71±0.21 versus 0.67±0.22, respectively; P=0.063) or mean solar day 5 and 6 (0.68±0.21 versus 0.67±0.22, respectively; P=0.65). Serum BUN increased in VLBW infants during their first days of life (repeated measure out ANOVA; P=0.004), and there was a statistically pregnant divergence (paired t-exam with Bonferroni correction) between serum BUN on day 2 and half-dozen of life (P=0.004, Figure 1b)
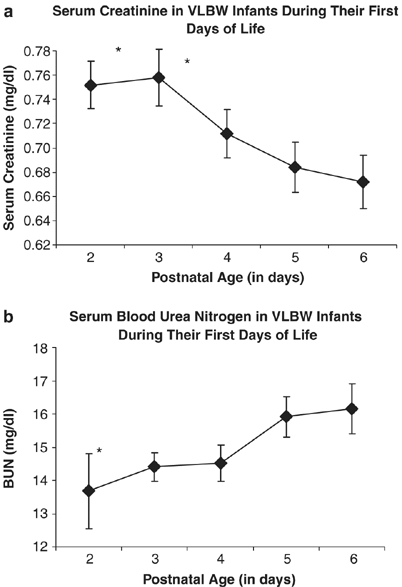
(a) SCr in VLBW infants during their first days of life. There is a decrease in SCr between mean solar day 2 and 6 of life (repeated measure ANOVA; P=0.004, due north=138). Data is presented as mean±due south.e. of the mean. *Denotes a statistically pregnant departure (P ⩽0.01) with SCr on 24-hour interval half-dozen of life. (b) Serum BUN in VLBW infants during their start days of life. There is an increase in serum BUN between twenty-four hour period 2 and vi of life (repeated measure ANOVA; P<0.004, due north=138). Information is presented as mean±south.e. of the mean. *Denotes a statistically meaning difference (P ⩽0.01) with Serum BUN on day 6 of life.
During the first days of life, there was a pregnant increment in intravenous fluid (IVF) intake (ANOVA; P<0.001, Effigy 2a) and urinary output between mean solar day ii and 6 of life (ANOVA; P=0.004, Figure 2b).
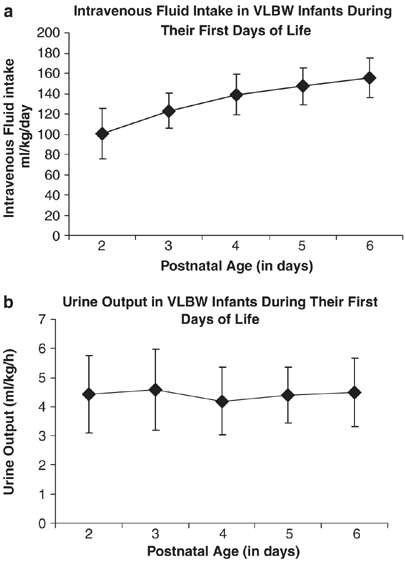
(a) IVF intake in VLBW Infants during their commencement days of life. In that location is an increase in IVF intake between day 2 and 6 of life (repeated measure ANOVA; P<0.001). (b) Urine output in VLBW infants during their showtime days of life. There is an increase in urinary output between day two and vi of life (repeated measure ANOVA; P=0.004).
In a subgroup assay there was no statistically pregnant decrease in SCr in infants <29 weeks GA (ANOVA; P=0.076), whereas there was a meaning subtract in SCr in infants 29 to 32 weeks GA during their offset days of life (ANOVA, P=0.016, Figure 3).
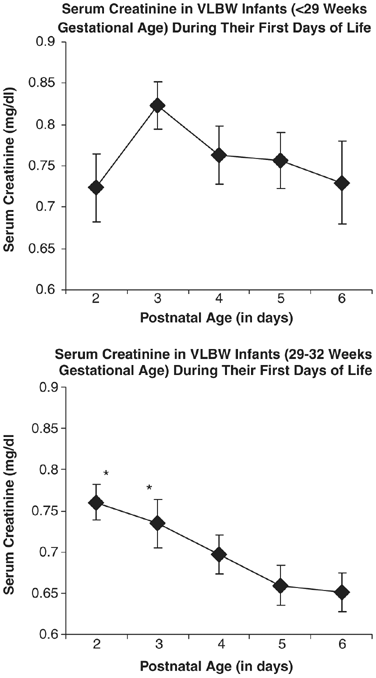
SCr in VLBW infants during their first days of life. There is no change in SCr between 24-hour interval 2 and vi of life in infants <29 weeks GA (repeated mensurate ANOVA; P=0.076), whereas in that location is a decrease in SCr between mean solar day 2 and 6 of life in infants 29 to 32 weeks GA (repeated measure ANOVA; P=0.016). *Denotes a statistically significant difference (P ⩽0.01) with SCr on day 6 of life.
In another subgroup analysis there was no statistically significant decrease in SCr in infants <1000?g (ANOVA; P=0.298), whereas there was a significant decrease in SCr in infants yard to 1500?1000 during their first days of life (ANOVA, P=0.004, Effigy iv).
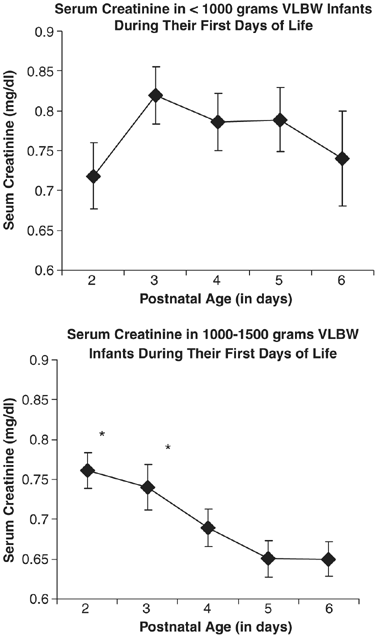
SCr in VLBW infants during their first week of life. In that location is no change in SCr between day 2 and half dozen of life in infants <1000?k BW (repeated measure ANOVA; P=0.298), whereas there is a decrease in SCr between day two and six of life in infants yard to 1500?one thousand BW (repeated measure out ANOVA; P=0.004). *Denotes a statistically significant difference (P ⩽0.01) with SCr on 24-hour interval 6 of life.
Following our offset observation that SCr reached a plateau betwixt the fourth and 6th day of life, we studied on the fifth twenty-four hours of life the relationships between SCr and GA, and SCr and BW. SCr on the fifth twenty-four hours of life was establish to decrease with increasing GA (Pearson correlation coefficient: −0.206 (P=0.05); Effigy v). On the fifth day of life SCr was plant besides to decrease with increasing BW (Pearson correlation coefficient: −0.236 (P=0.05). Figure 6).
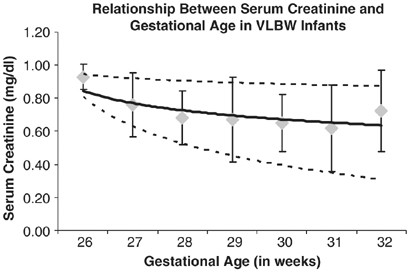
Relationship between SCr (mg/dl) and GA (weeks) in VLBW infants. There is a decrease in SCr betwixt ⩽26 and 32 weeks GA, on day 5 of life. Pearson Correlation coefficient: −0.192 (P=0.05, north=138). SCr values are presented in hateful±s.d. and likewise in 10th, 50th and 90th percentiles. Diamonds represent the mean±southward.d. values. The solid line represents the 50th percentile, and the dashed lines represent the tenth and 90th percentile.
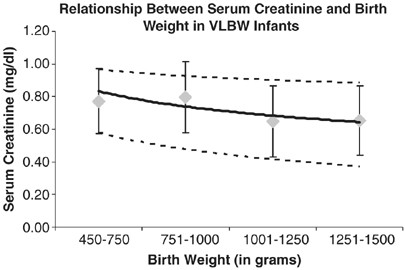
Relationship between SCr (mg/dl) and BW (grams) in VLBW infants. In that location is a subtract in SCr between 450 to 750?k and 1251 to 1500?thou groups. Pearson correlation coefficient: −0.236 (P=0.05; n=138). SCr values are presented in mean±due south.d. and also in 10th, 50th and 90th percentiles. Diamonds correspond the mean±southward.d. values. The solid line represents the 50th percentile, and the dashed lines correspond the tenth and 90th percentile.
Table 2 shows patients characteristics on their fifth solar day of life.
Among our patients, 89% (123/138) received gentamicin, 48% (66/138) received xanthines (aminophylline, and or caffeine), and 21% (29/138) remained mechanically ventilated (intubated) or on CPAP during the study menses. To adjust for the use of gentamicin, xanthines and mechanical ventilation/CPAP equally possible misreckoning factors that tin can alter SCr levels; a logistic regression analysis was conducted. A ⩾10% decrease in SCr (between day 2 and 6) was chosen as the dependent variable and utilize of gentamicin, xanthines or mechanical ventilation/CPAP every bit independent variables. At that place was no statically significant consequence of gentamicin, xanthines or mechanical ventilation/CPAP on the alter of SCr betwixt day ii and six of life (Tabular array 3). The decrease by ⩾10% of SCr was chosen because SCr dropped from 0.75 on day 2 of life to 0.65 on mean solar day 6 of life (an guess decrease of 10%).
To decide if mechanical ventilation/CPAP in younger infants (<29 weeks GA) is contributing to the college SCr levels at day 6 of life a subgroup assay was conducted. L-six % (13/23) of ventilated infants on day two of life remained on mechanical ventilation/CPAP on day 6 of life (in infants <29 weeks GA) versus 42% (16/38) of ventilated infants on day 2 of life remained on mechanical ventilation/CPAP on day 6 of life (in infants ⩾29 weeks GA; P=0.27). There was no meaning difference in the percent of ventilated or treated with CPAP patients among younger or older infants during the study period.
Discussion
Nosotros have shown in a big cohort of VLBW (459 to 1493?g) infants that SCr is elevated on the 2nd day of life, and decreases postnatally to reach a plateau between the quaternary and sixth day of life. However, in a subgroup analysis nosotros found that SCr does not subtract significantly during the commencement 6 days of life in infants <29 weeks GA and <1000?grand BW. We have too shown that infants' SCr (on the fifth 24-hour interval of life) decreases with advancing GA and BW.
The high morbidity of VLBW infants during the first 2 days of life, and exposure to multiple agents that might impair renal function, get in very difficult to establish normal reference values of SCr during the first days of life. During the first 2 days of life the high level of SCr in newborn infants has been attributed to a combination of maternal creatinine levels,1 immaturity of the glomerular filtration, and an increased tubular reabsorption of creatinine due to a possible back-menstruum of creatinine across leaky immature tubular and vascular structures.two Others accept besides reported reduced GFR values during the commencement 48?h of life secondary to the inability of premature kidneys to clear loftier SCr values.iii, fourteen To determine the relationship between SCr and GA, and SCr and BW in VLBW infants, SCr values of all VLBW infants were studied during their first days of life. The fifth 24-hour interval of life was chosen to study the human relationship betwixt SCr and GA or BW because SCr reached a plateau between the fourth and sixth solar day of life. Our findings are consequent with others; Bueva et al. fourteen accept shown in xi patients (1001 to 1500?m) a decrease in SCr between day 1 to 2 and 8 to 9 (from 95±5 to 64±v?μmol/50, respectively).
In a modest number of patients divided between ii groups of <xxx weeks GA and 31 to 34 weeks GA, Vanpee et al. 8 take shown that postnatal evolution of renal function is also related to GA, and postnatal development of renal part is slower in premature infants than in full term infants. These authors have shown that: from the first to the 5th postnatal week, creatinine clearance (in ml/min/1.73?grandtwo) increased from 10 to 20 in infants <xxx weeks GA at nascence. Whereas, creatinine clearance increased from 15 to xxx in infants 31 to 34 calendar week GA at nascency. Their findings are besides consistent with ours. In our written report, nosotros did not measure GFR in VLBW infants, however, we plant in infants <29 weeks GA and <k?thousand BW that SCr remained elevated during the outset days of life most probably secondary to a low creatinine clearance in these extremely premature infants.
The serum BUN as well increased during the offset week of life in our patients almost probably secondary to the increase in protein intake betwixt mean solar day 2 and vi of life. On average our patients reached an intake of 2?m/kg/day of poly peptide on their fifth day of life. IVF intake and urinary output increased during the first days of life every bit expected, secondary to fluid restriction during the first few days of life. Some other explanation for the subtract in creatinine along with an increase in BUN could be related to an insufficient fluid or caloric intake in our patients or could be related to a progressive decrease in tubular back leak of creatinine (a hypothesis that cannot exist tested without measurement of GFR).
We have shown in our study that SCr decreases with advancing GA. Our findings are consequent with previous findings of Bueva et al. 14 who have shown that plasma creatinine concentration is significantly college in preterm infants compared to term infants between the first and 2d day of life, and that creatinine clearance correlates with GA. In their study these authors assessed 66 term and preterm infants (1000 to 2500?g BW of which merely eleven patients were 1001 to 1500?g), whereas in our study we evaluated 136 infants 25 to 32 weeks GA (<1500?g). In some other report, Gallini et al. 6 accept shown a correlation between serum SCr and postnatal age in 83 preterm infants <32 weeks GA. In their study there was no divergence in SCr among infants of different GA at birth, but these authors found an changed correlation between SCr and GA from the third day of life to the 5th week. During the first calendar week of life the maximum value of SCr was significantly college in the group of infants <27 weeks GA than infants who were 27 to 28 weeks, 29 to 30 weeks and 31 to 32 weeks. These findings are consistent with ours; we establish that SCr, in infants <29 weeks GA and <1000?g BW, does not decrease significantly during the first calendar week of life in comparison to infants 29 to 32 weeks GA and 1000 to 1500?g BW, respectively.
At that place are limitations to our study. Nosotros conducted a retrospective review of our patients' medical records; we did not mensurate creatinine clearance in order to decide if there is whatever correlation between creatinine clearance and GA or BW. Nosotros did not have prenatal medical records bachelor for review. Any prenatal exposure to nephrotoxic medications such as prostaglandin inhibitors could have contradistinct the results of our report. Another limitation to our study is the possibility of the presence of a silent PDA that could have affected renal perfusion and function.xv We excluded patients with PDA who were symptomatic and who had an echocardiogram to confirm the diagnosis. We did not have cardiac echocardiograms carried out routinely to exclude patients with silent PDA. We also excluded patients from our study who were on a high ventilator settings (such equally on the oscillator), but we did non exclude patients who were on conventional mechanical ventilation. Whatsoever grade of mechanical ventilation that increases intrathoracic pressure may impair venous return and renal perfusion.15 However, in our logistic regression analysis mechanical ventilation or CPAP did non have any statistically significant issue on SCr during the study menstruum. Also, in a subgroup analysis of our patients we did not find whatsoever difference in the per centum of patients who remained on mechanical ventilation/CPAP during the entire study period between infants younger or older than 29 weeks. It volition be difficult to recruit VLBW infants during their first days of life who are not in respiratory distress and on mechanical ventilation. Prospective, long-term studies are needed to explore the maturation of renal function in premature infants and to determine if there is a delay in renal maturation and part that extends beyond the neonatal menses to infancy, childhood and or adulthood. With advancing engineering, younger premature infants (<25 calendar week GA) are surviving, time to come studies are also necessary to determine renal function and maturation at this very young age group.
We conclude that in VLBW infants SCr decreases during the showtime days of life to accomplish a plateau between the fourth and sixth day of life (on average on the fifth day) most probably reflecting the infants own SCr than the mothers. However, in infants younger than 29 weeks GA or smaller than 1000?1000 at birth at that place is a filibuster in the decrease of their SCr that extends beyond the beginning 6 days of life. We likewise conclude that during the first days of life (on the fifth solar day of life), and in VLBW infants SCr decreases with advancing GA and BW.
References
-
Chevalier RL . Developmental renal physiology of the depression nascency weight pre-term newborn. J Urol 1996; 156: 714–719.
-
Guignard JP, Drukker A . Why practise newborn infants take a loftier plasma creatinine? Pediatrics 1999; 103(4): e49.
-
Miall LS, Henderson MJ, Turner AJ, Brownlee KG, Brocklebanck JT, Newell SJ et al. Plasma creatinine rises dramatically in the first 48?h of life in preterm infants. Pediatrics 1999; 104(half dozen): 1–4.
-
Lao TT, Loong EP, Mentum RK, Lam YM . Renal function in the newborn. Newborn creatinine related to birth weight, maturity and maternal creatinine. Gynecol Obstet Invest 1989; 28(2): 70–72.
-
Sonntag J, Prankel B, Waltz Due south . Serum creatinine concentration, urinary creatinine excretion and creatinine clearance during the first 9 weeks in preterm infants with a nascence weight below 1500?g. Eur J Pediatr 1996; 155(9): 815–819.
-
Gallini F, Maggio L, Romagnoli C, Marrocco G, Tortorolo One thousand . Progression of renal office in pretern neonates with gestational historic period ⩽32 weeks. Pediatr Nephrol 2000; 15: 119–124.
-
van der Heijden AJ, Grose WF, Ambagtsheer JJ, Provoost AP, Wolff ED, Sauer PJ . Glomerular filtration rate in the preterm infant: the relation to gestational and postnatal age. Eur J Pediatr 1988; 148(1): 24–28.
-
Vampee Thou, Herin R, Zetterstrom R, Aperia A . Postnatal development of renal function in very low birthweight infants. Acta Paediatr Scand 1988; 77: 191–197.
-
Schwartz GJ, Brion LP, Spitzer A . The use of plasma creatinine concentration for estimating glomerular filtration charge per unit in infants, children, and adolescents. Pediatr Clin Northward Am 1987; 34(iii): 571–590.
-
Zacchello G, Bondio M, Saia OS, Largaiolli K, Vedaldi R, Rubaltelli FF . Uncomplicated approximate of creatinine clearance from plasma creatinine in neonates. Arch Dis Child 1982; 57(4): 297–300.
-
Brion LP, Fleischman AR, McCarton C, Schwartz GJ . A elementary estimate of glomerular filtration rate in low birth weight infants during the first twelvemonth of life: noninvasive cess of body composition and growth. J Pediatr 1986; 109(4): 698–707.
-
Cicero FM, Okay Y, Araujo RJL . Relationship between plasma creatinine concentration and glomerular filtration in preterm newborn infants. Rev Hosp Clin Fac Med Sao Paulo 1999; 54(4): 121–126.
-
www.beckmancoulter.com.
-
Bueva A, Guignard JP . Renal function in preterm neonates. Pediatr Res 1994; 36(5): 572–577.
-
Vampee M, Ergander U, Herin P, Aperia A . Renal function in sick, very depression-birth-weight infants. Acta Paediatr 1993; 82: 714–718.
Author information
Affiliations
Respective author
Additional data
Financial supported: none.
Rights and permissions
About this commodity
Cite this article
Auron, A., Mhanna, M. Serum creatinine in very low birth weight infants during their first days of life. J Perinatol 26, 755–760 (2006). https://doi.org/ten.1038/sj.jp.7211604
-
Received:
-
Revised:
-
Accustomed:
-
Published:
-
Result Date:
-
DOI : https://doi.org/x.1038/sj.jp.7211604
Keywords
- gestational age
- very low birth weight
- serum creatinine
- postnatal age
- infants
- neonatal intensive care unit
Farther reading
Source: https://www.nature.com/articles/7211604
0 Response to "What Does a Low Creatinine Level Mean in a Premature Baby"
Post a Comment